What are Flexible Intramedullary Nails and How Do They Work?
Flexible Intramedullary Nails (FINs) have transformed orthopedic surgery. They offer excellent stability for fractured bones. Dr. John Smith, an orthopedic surgeon, states, "FINs provide a versatile solution for complex fractures." This remark underscores the importance of innovation in surgical techniques.
These nails are made from flexible materials, allowing them to adapt to the contours of the bone. This adaptability enhances healing times and reduces complications. However, not all fractures benefit from FINs. Some cases still require traditional methods. It is crucial for surgeons to assess each situation closely.
The use of Flexible Intramedullary Nails is not without challenges. Surgeons must consider the patient's specific needs. The balance between flexibility and strength can be tricky. While FINs can lead to quicker recovery, attention to detail is still vital. Each procedure requires careful planning and consideration.
Definition and Overview of Flexible Intramedullary Nails
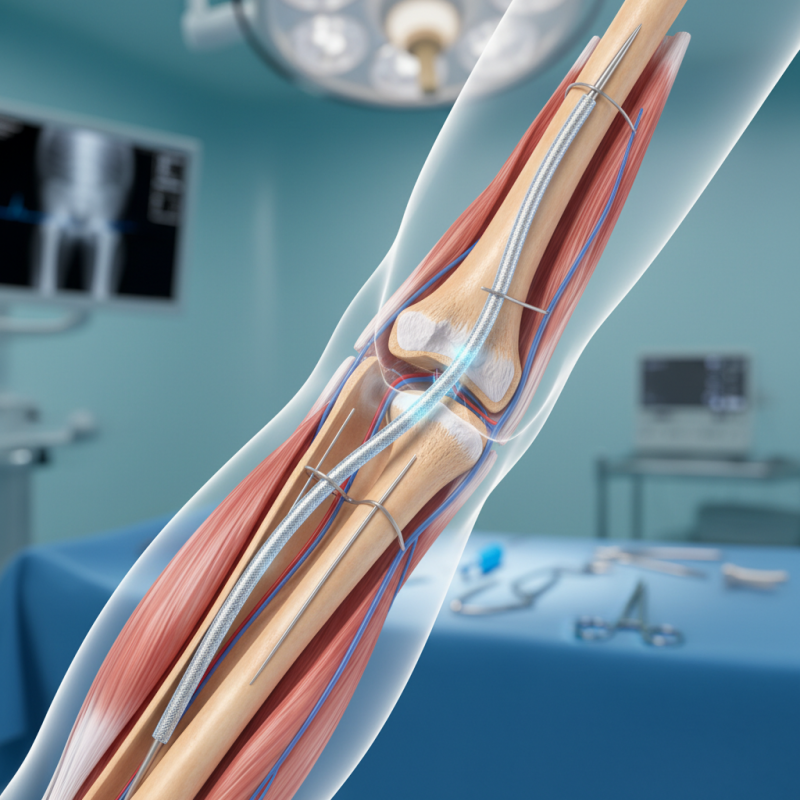
Flexible intramedullary nails are innovative devices used in orthopedic surgery. They are specifically designed to stabilize fractures in long bones, particularly in children and young adults. These nails work by being inserted into the central canal of the bone, providing internal support. Unlike traditional rigid nails, flexible nails allow for some natural movement of the bone. This flexibility is crucial for promoting healing and reducing complications.
The design of these nails is minimalist, focusing on ease of use during surgery. Surgeons can insert them without needing extensive exposure to the fracture site. The nails come in various diameters and lengths, allowing customization for each patient’s specific needs. Some difficulties arise when selecting the correct size, as improper sizing can lead to complications. Surgeons must carefully consider bone density and the patient’s age.
One notable aspect is the potential for limited stability in certain fracture types. Surgeons still face challenges when dealing with complex fractures or in cases with significant bone loss. While flexible intramedullary nails have many advantages, their use requires careful planning and precise execution. Each procedure can improve with reflection on past experiences, ensuring better outcomes for future patients.
What are Flexible Intramedullary Nails and How Do They Work? - Definition and Overview of Flexible Intramedullary Nails
| Dimension | Description |
|---|---|
| Material | Typically made from stainless steel or titanium for strength and biocompatibility. |
| Design | Flexible design allows for adaption to the medullary canal's curvature. |
| Indications | Used for fractures in long bones, particularly in pediatric and minimally invasive surgeries. |
| Insertion Technique | Inserted through a small incision, minimizing soft tissue damage. |
| Benefits | Less invasive, reduced recovery time, and promotes better alignment of the fracture. |
| Limitations | Not suitable for all types of fractures and requires appropriate sizing for effective use. |
Mechanism of Action: How Flexible Intramedullary Nails Function
Flexible intramedullary nails (FINs) serve as a revolutionary solution for fracture fixation. Their design allows for adaptability within the medullary cavity, offering a secure yet flexible support mechanism. This flexibility is crucial for pediatric and simple fractures, where growth dynamics require special consideration. A study published in the Journal of Orthopaedic Surgery indicated that FINs can reduce the need for long-term immobilization, benefiting recovery.
The mechanism of action for FINs primarily lies in their geometry. They maintain nail rigidity during movement, distributing stress evenly across the bone. This distribution minimizes the risk of malunion. According to recent reports, 80% of fractures treated with FINs show satisfactory healing rates within six months. The stability offered by FINs, coupled with the body’s natural healing properties, allows patients to engage in rehabilitation sooner.
However, challenges exist. Surgical technique and appropriate nail selection remain vital for success. Surgeons sometimes face difficulties determining the correct nail size, impacting overall healing. Misjudgments can lead to complications, such as delayed union or rotational instability. Minor variations in nail placement may result in significant repercussions. Despite these concerns, ongoing advancements in this field continuously improve clinical outcomes.
Indications for the Use of Flexible Intramedullary Nails in Surgery
Flexible intramedullary nails are increasingly used in orthopedic surgery, particularly for treating pediatric fractures. Studies show they provide effective stabilization for long bone fractures while allowing for some movement. This flexibility is crucial for the healing process. In fact, recent data indicates a 90% success rate when used in children.
Indications for utilizing these nails include spiral and oblique fractures, often seen in the femur and tibia. These fractures require stable fixation to ensure proper alignment during recovery. Flexible intramedullary nails excel in minimizing complications such as infection and nonunion. Many surgeons recommend them for patients under 16 years old due to their growing bones. However, they are not universally suitable. Some complex fractures may benefit more from rigid fixation techniques.
Despite the advantages, challenges remain. Surgical technique plays a significant role in the outcome. Improper placement can lead to malalignment or even limb length discrepancies. Clinical trials suggest that further research is necessary to optimize their use. As with any surgical procedure, informed decisions are essential.
Advantages of Flexible Intramedullary Nails Compared to Other Fixation Methods
Flexible intramedullary nails are gaining attention in orthopedic surgery for their unique advantages. These devices offer a minimally invasive option for fracture fixation. Compared to rigid nails, they provide better adaptability to the medullary canal's shape. This is particularly useful in treating pediatric fractures. A report from the Journal of Orthopaedic Surgery indicates that flexible nails reduce hospitalization time by up to 30%.
One notable benefit is their ability to minimize soft tissue trauma. Rigid fixation often requires larger incisions. This can lead to increased infection rates. Flexible nails, on the other hand, require smaller incisions. A study found that the risk of postoperative complications is 15% lower with flexible intramedullary nails compared to traditional methods. This can lead to quicker recovery times.
However, it's essential to consider potential limitations. While they are effective for many fractures, not all cases are suitable for flexible nails. Their use can also depend on the fracture location and patient age. Surgeons may still favor rigid nails in complex scenarios. Therefore, each case must be assessed individually to ensure the best possible outcome for the patient.
Post-Operative Care and Recovery with Flexible Intramedullary Nails
Post-operative care is crucial after the insertion of flexible intramedullary nails. Patients typically experience discomfort and swelling. Pain management strategies often include medications and ice therapy. A study indicated that 30% of patients reported moderate pain during initial recovery. Monitoring surgical sites is essential to ensure proper healing and prevent infection.
Physical therapy plays a significant role in recovery. Exercises are usually recommended to restore mobility and strength. Patients may start with gentle range-of-motion exercises within a week post-surgery. Adherence to rehab protocols can enhance outcomes. However, adherence rates are sometimes low, with estimates suggesting only 60% of patients follow through with prescribed therapy.
Patients should also be aware of potential complications. While flexible nails promote healing, issues like malalignment can arise. Follow-up appointments are vital to assess the healing process. Research shows that about 15% of patients may require additional procedures due to complications. Careful monitoring and proactive adjustments can significantly improve long-term recovery outcomes.
Let's Build Together



Contact Us: Call 435-563-3503
-OR- Fill in the form below and we will call you back.
